Autism and Autism Services with Indigenous Families and Children in the Settler-Colonial Context of Canada: A Critical Scoping Review
Aliso J. Gerlach, MSc(OT), PhDh
Asssistant Professor, School of Child and Youth Care
Faculty of Human and Social Development
University of Victoria
alisongerlach [at] uvic [dot] ca
Amarens Mattiesen, MA (CYC)
PhD Candidate, School of Child and Youth Care
Faculty of Human and Social Development
University of Victoria
amarensm [at] uvic [dot] ca
Fiona J. Moola, PhD
Assistant Professor
School of Early Childhood Studies, Ryerson University, Toronto, ON, Canada
Holland Bloorview Kids Rehabilitation Hospital, Toronto, ON, Canada
Dalla Lana School of Public Health, University of Toronto, Toronto, ON, Canada
Rehabilitation Sciences Institute, University of Toronto, Toronto, ON, Canada
fiona [dot] moola [at] ryerson [dot] ca
Jackie Watts
Provincial Advisor
Aboriginal Supported Child Development Programs of British Columbia
Victoria, Brisih Columbia
advisor [dot] ascdp [at] bcaafc [dot] com
Abstract
In Canada, Indigenous families and children experience structurally-rooted marginalization due to longstanding and ongoing histories of colonization and discrimination. Indigenous children with autism spectrum disorder (ASD) are currently underrepresented in literature and databases on ASD in Canada, raising concerns about their equitable access to related services and optimal health outcomes. This critical scoping review maps out existing and emerging themes in literature pertaining to ASD and the provision of ASD services with Indigenous children and families in Canada. No previous reviews of literature have focused exclusively on ASD among Indigenous children in Canada. A literature search conducted across eight databases between 2011 and 2021 resulted in 362 potentially relevant publications, of which 19 met our inclusion criteria. Findings point to a clear lack of data on ASD and unmet health, social, and educational service needs among Indigenous children with ASD in Canada. ASD is also frequently discussed through a Western, deficit and medical discourse. The main contributors to the lack of data and unmet service needs relate to the historical positioning of colonial oppression, stigma, an overrepresentation of fetal alcohol spectrum disorder (FASD), lack of funding, and concerns about standardized diagnostic and assessment tools, and social determinants of health. Recommendations for policy, practice and research concerning Indigenous children with ASD are proposed.
Keywords: Equity; intersectionality; Jordan's Principle; inequities
Introduction
The increasing worldwide prevalence of autism spectrum disorder (herein called ‘autism) supports claims of an ‘autism epidemic’ (Chiarotti & Venerosi, 2020). In Canada, it has been estimated that approximately one in 66 children between five and 17 years of age has autism (Public Health Agency of Canada, 2018). Autism is an early onset, heterogenous neurodevelopmental disorder, characterized by specific cognitive features (Lord et al., 2020). The specific diagnostic criteria of autism, as outlined in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-V) involves deficits in social communication and interaction, as well as restricted and repetitive patterns of behavior, interests, or activities (American Psychiatric Association, 2013).
Access to early child development (ECD) and intervention, prior to entering the educational system, is recognized as being essential to enhancing outcomes for children with autism (Masi et al., 2021; Vivanti, 2012). In many jurisdictions across Canada, referral to, and early assessment and diagnosis of ASD by a pediatric specialist or team is the typical gatekeeper for parents[1] to be able to access specific funding, supports and services for their children. ECD and intervention for children with ASD can include a range of different services including speech language therapy, physiotherapy, occupational therapy and behavioral intervention. For example, in British Columbia (BC), a medically-confirmed diagnosis of autism with preschool-aged children can provide parents’ access up to $22,000 per year towards their child’s support needs (Luckow, 2019). Although it is possible to detect autism as early as two years of age (Zwaigenbaum et al., 2019), the mean age of diagnosis for autism in the general child population in Canada is four to five years of age (Public Health Agency of Canada, 2018).
In the colonial nation of Canada, Indigenous communities and families remain an incredibly diverse population, with distinct histories, languages and cultures and rich and complex knowledge systems that are foundational determinants of health for Indigenous children (Halseth & Greenwood, 2019). Nonetheless, historical and ongoing colonial relations of power, continue to have direct, unjust and detrimental impacts on Indigenous children’s early health, development and life trajectories (Greenwood et al., 2015). Indigenous families’ experiences of intergenerational and ancestral familial trauma from government-sanctioned forms of structural violence; historically in the form of the residential school system (Truth and Reconciliation Commission of Canada, 2015) and today, through child welfare systems that continue to remove Indigenous children from their families at rates incommensurate with the population, shape Indigenous children’s health and life chances and their parents’ decision-making about accessing ECD services (Gerlach, Browne, Sinha, et al., 2017; McKenzie et al., 2016).
Indigenous parents’ equitable access to ECD and intervention can also be influenced by everyday lived and anticipated experiences of racism, dismissal and discrimination, including in their encounters with the Canadian healthcare, ECD and children’s disability systems (Allan & Smylie, 2015; Gerlach, Browne, & Greenwood, 2017; Ineese-Nash et al., 2018; Wright et al., 2019). The colonial construction of ‘disability’ and its underlying assumptions of ‘(ab)normalcy’ may also influence the accessibility and efficacy of early intervention and disability services with Indigenous parents who may hold their own distinct views of child rearing, development and neurodiversity (Ineese-Nash, 2020; Ineese-Nash et al., 2018).
Jordan’s Principle represents a child-first principle named in honour of Jordan River Anderson from Norway House Cree Nation in Manitoba. Jordan encountered tragic delays in services that would otherwise have allowed him to experience life outside a hospital setting before his death. Unanimously endorsed by the House of Commons in 2007, Jordan’s Principle is intended to prevent denials, delays, or disruptions in services for Indigenous children due to jurisdictional disputes. However, a growing recognition exists that the federal government response “does not reflect the vision of Jordan’s Principle advanced by First Nations and endorsed by the House of Commons” (Sinha & Wong, 2015, p. 62).
Theoretical Framework: In terms of Indigenous families’ access to the autism system, the authors of this paper came together over a shared concern about an apparent lack of Indigenous-focused autism data and research in Canada. Using a critical scoping review methodology, this paper provides an overview and critical analysis of recurring themes in the literature on autism and autism services with Indigenous children and families in Canada with the goal of informing emerging practice and identifying future research priorities. We adopted an overall critical approach to the data in an effort to deepen our analysis. This included the use of critical frameworks such as intersectionality theory (Hill, Collins & Bilge, 2016; Crenshaw, 1991) as well as critical disability studies (Oliver, 2013). Such critical thinking has allowed us to be aware of how the literature may perpetuate power imbalances and reproduce dominant assumptions about Indigenous children with autism.
Current Study
This scoping review of both peer-reviewed and grey literature aimed to identify and critically analyze key themes on Indigenous peoples with autism in Canada in order to inform emerging practice and research priorities. The original catalyst for this scoping review was several meetings in 2019 and 2020 between community partner and co-author Jackie Watts and lead author Alison Gerlach about the lack of knowledge and resources currently available to guide frontline, Indigenous ECD providers supporting Indigenous families across BC whose children may have/have autism. Watts is a member of the Tseshaht First Nation on Vancouver Island and the Provincial Advisor for 57 ‘Aboriginal Supported Child Development Programs’ (ASCDP) across BC which provides supports for young Indigenous children with developmental delays and disabilities so that they can be fully included in childcare settings and their communities (see - https://www.ascdp.bc.ca/). Watts has many years in the Indigenous early years sector in BC. Gerlach is a White-settler immigrant with British ancestry, who has 22 years of experience as a community-based, pediatric occupational therapist and researcher with Indigenous and mainstream early child development stakeholders in BC, and has known Watts and collaborated on committees and projects involving ASCDP for many years. Watts and Gerlach decided that the first step in addressing this need was to find out what had already been written about Indigenous perspectives on autism in Canada. In deciding to use a scoping review methodology, Gerlach invited co-author Moola to join the study. Fiona Moola is a first-generation Canadian settler and woman of colour of South African descent, who has experience, as a childhood disability researcher, of conducting scoping reviews. Gerlach obtained a small research grant from the Human and Social Development Faculty at the University of Victoria (UVic), which funded a graduate research assistant, Matthiesen, to conduct the literature search and be a co-author. Amarens Matthiesen is a second-generation White settler of Dutch and Danish descent. She is a doctoral candidate at the University of Victoria and an experienced child life specialist.
Methodology
A scoping review methodology was employed in order to map the extant published literature on autism in Indigenous populations in Canada. In contrast to systematic literature reviews, scoping reviews allow for a broader exploration of a topic area by incorporating all relevant literature types and study designs (Helou et al., 2020). By capturing “the breadth and depth of a field” (Levac et al. 2010, p. 1), a scoping review methodology aligned well with the broad nature of our topic of interest and desire to capture a range of publication types and study designs. The critical intersectional lens that informed our work supported the authors in troubling, critiquing and elucidating assumptions in the evidence (Ellis et al., 2020; King et al., 2020; Schwellnus et al., 2015; van der Kleij & Lipnevich, 2021; Webster et al., 2017). Our search included peer-reviewed articles and grey literature (including government reports, news articles, theses, and organization/association reports) and followed a five-step scoping review framework proposed by Levac et al. (2010), as outlined below.
Step 1: Identification of the Research Questions
The authors co-created the following research questions to guide the scoping review:
- What is known about autism diagnosis and prevalence in Indigenous communities in Canada?
- What is known about how autism is perceived by Indigenous peoples in Canada?
- What is known about the intersections of autism, the child protection system in Canada and Indigenous communities?
Step 2: Identification of Relevant Studies
The authors refined the search strategy to identify literature on autism and autism services for Indigenous children and families in Canada. This process included the selection of keywords to create a total of five search strings which captured the main concepts of interest reflected in our research questions. Keywords were subsequently refined following multiple rounds of discussion amongst the authors. An academic research librarian was consulted to ensure the appropriateness of the scope and efficacy of keywords and search strings. Search techniques included the use of Boolean terms “AND/OR” to define the relationships between keywords and truncation (*) to account for terms with multiple endings. An overview of the keywords entered into the respective search strings is attached in Appendix A.
Each search string was combined through the Boolean term “AND” and adapted for use in the search engine of multiple databases. The Google Scholar search engine functionality and word limit forced a shortened search string to be entered. In consultation with a librarian at the University of Victoria, the search focused on eight databases: PsycINFO; Education Resources Information Center (ERIC); Web of Science; PubMed; Cochrane Library; Cumulative Index to Nursing and Allied Health Literature (CINAHL) and Google scholar. Google search engine was also used to identify grey literature in which the first seven pages of results were included as subsequent pages diminished in relevance. Reference lists of articles were also scanned to identify additional relevant literature (Levac et al., 2010).
Step 3: Study Selection
An iterative team approach was taken to selecting pertinent studies for inclusion (Levac et al., 2010). During this stage, Matthiesen gained familiarity with the literature by completing multiple rounds of reading the literature on autism services for Indigenous children and families in Canada. The first three authors subsequently met to discuss decisions surrounding study inclusion and exclusion criteria (Levac et al., 2010), as summarized in Table 2. Given the anticipated paucity of literature on this topic, the search was not restricted by date of publication or research design. Further consensus on inclusion criteria was reached by frequent discussion amongst the authors.
Table 2. Inclusion and Exclusion Criteria
| Criterion | Inclusion | Exclusion |
|---|---|---|
| Language | English | Non-English |
| Study focus | Provision of any type of health, social, child welfare and/or community-based support service(s) | Not focused on the provision of health, social and/or community-based support service |
| Population | Indigenous(including Indigenous (including Métis, Inuit or First Nations) children (0-14 years) and/or youth (15-24 years) with ASD | Non-Indigenous children and/or youth with ASD |
| Location | Canada | Not focused on Canada |
Matthiesen started screening the literature using a three-step process: (1) The inclusion criteria were applied to the titles and abstracts of the retrieved studies. When titles or abstracts did not provide enough clarity on whether inclusion criteria were met, they were automatically included in the second stage of screening. (2) Studies were read in full to further evaluate their alignment with the research questions and inclusion criteria. (3) All authors collectively reviewed and reached consensus on the final data set.
Step 4: Charting the Data
The authors collectively determined which variables to extract in order to answer the research questions (Levac et al., 2010). Matthiesen used a Microsoft Word (Microsoft Corp.) spreadsheet to summarize data according to the author(s), year and type of publication, study aims, methodological considerations and location, sample characteristics, key findings, and recommendations for practice and/or future research. An assessment tool to grade the quality of evidence was not employed as the aim of our review was to describe the extent of the literature (Arksey & O’Malley, 2005).
Step 5: Coding and Thematic Analysis
Matthiesen used a code book co-developed with Gerlach and Hunter and informed by a preliminary scan of the literature. All authors subsequently collaborated on refining the preliminary coding which was then used to code the findings. The coded findings formed the basis for collaboration on thematic analysis of the data (Clarke & Braun, 2017; Finkelstein et al., 2021; Moola et al., 2020). Over the course of several months, collaborative thematic analysis included visual mapping and close and ongoing consultation amongst all authors until agreement was reached on the overarching themes.
Step 6: Stakeholder Consultation
As an essential component of a scoping review methodology (Levac et al., 2010), the catalyst for this review and the focus on Canada was initiated by community partner Watts, to address her concerns about the need for increased knowledge on autism and autism services with Indigenous children and families. In the spring and summer of 2021, further consultation by the first three authors and Watts guided a final framing of the research questions, results and analysis of the literature search, and input on a preliminary framing of the findings and their potential implications.
Results
The results of the search process are summarized in Figure 2. The initial keyword search resulted in a total of 362 publications. After removing 55 duplicates, full-text reviews were performed on 100 publications resulting in 19 articles that met all inclusion criteria (Table 3).
Figure 1: Flow Chart of Search Strategy
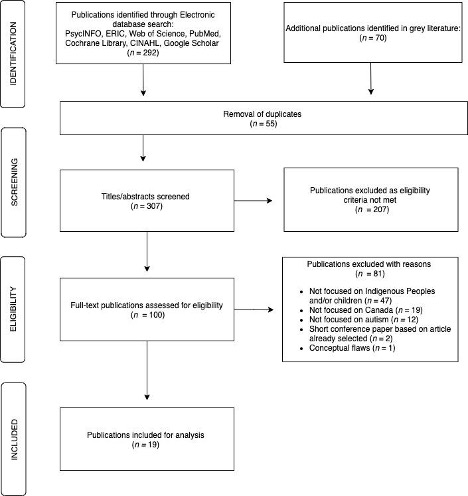
Table 3. Final Articles that met the Inclusion Criteria in Alphabetical Order (N=19)
| Author and Date | Title |
|---|---|
| 1. Burstyn et al. (2010) | Autism spectrum disorders, maternal characteristics and obstetric complications among singletons born in AB |
| 2.Canadian Autism Partnership Project (2016) | Better together: The case for a Canadian Autism partnership |
| 3. Di Pietro & Illes (2014) | Disparities in Canadian Indigenous Health Research on Neurodevelopmental Disorders |
| 4. Di Pietro & Illes (2016) | Closing Gaps: Strength-Based Approaches to Research with Aboriginal Children with Neurodevelopmental Disorders |
| 5. Government of Canada (2018) | Report on the National Autism Spectrum Disorder Surveillance System |
| 6. Hiebert-Murphy et al. (2008) | Patterns of entry to community‐based services for families with children with developmental disabilities: implications for social work practice |
| 7. Inman (2019) | Absence and epidemic: Autism and FASD in Indigenous populations in Canada |
| 8. Leitch (2007) | Reaching for the top: A report by the Advisor on Health Children & Youth |
| 9. Lindblom (2013) | Possible educational implications of the underdiagnosis of autism spectrum disorders, ASDs, of aboriginal children in BC |
| 10. Lindblom (2014a) | Under-detection of autism among First Nations children in BC |
| 11. Lindblom (2014b) | How to listen and give voice to First Nations children in BC diagnosed with Autism Spectrum Disorder– ethnography in practice |
| 12. Lindblom (2017a) | It gives them a place to be proud’–Music and social inclusion. Two cases of young First Nations people diagnosed with autism in BC |
| 13. Lindblom (2017b) | Stepping out of the shadows of Colonialism to the beat of the drum: The meaning of music for 5 First Nations children with autism in BC |
| 14. Luckow (2019) | Autism study aims to help Indigenous families procure services |
| 15. Manitoba First Nations Engagement (2017) | Keewaywin Engagement Manitoba First Nations Child and Family Services Reform |
| 16. Ouellette-Kuntz et al. (2006) | Prevalence of Pervasive Developmental Disorders in Two Canadian Provinces |
| 17. Shochet et al. (2020) | Psychosocial resources developed and trialed for Indigenous people with autism spectrum disorder and their caregivers: A systematic review and catalogue |
| 18. Stephanow (2019) | New research projects aim to improve autism supports on First Nations |
| 19. Woodgate (2013) | Understanding the Disability Trajectory of First Nations Families of Children with Disabilities: Advancing Jordan’s Principle |
Literature Characteristics
As summarized in Table 4, literature that met the inclusion criteria varied in type of publication, research design, and study population and context.
Table 4. Literature Characteristics
Peer-reviewed Literature
| Qualitative | 3 |
| Quantitative | 2 |
| Systematic literature review | 1 |
| Unspecified literature review | 2 |
| Conference papers | 2 |
Grey Literature
| Government and/or NGO report | 5 |
| News Article | 2 |
| Discussion/conceptual paper | 1 |
| Doctoral dissertation | 1 |
Geographic Location
| Multiple provinces/territories | 9 |
| British Columbia | 5 |
| Manitoba | 3 |
| Saskatchewan | 1 |
| Alberta | 1 |
Findings
Collaborative analysis of the findings by the authors resulted in the identification of several recurring and inter-related themes. A critical, intersectional lens was used to analyze the findings and explore their practice and research implications.
The Hegemony[2] of a Medical Worldview
Not surprisingly perhaps, the literature reviewed on autism and Indigenous children frequently defaulted to a medical worldview centred on a diagnostic criteria of autism spectrum disorder, as outlined in the aforementioned DSM-V, developed by the American Psychiatric Association (2013) (Lindblom 2013, 2014a; Government of Canada, 2018; Ouellette-Kuntz et al., 2006; Shochet et al., 2020). Consistent with the tendency of a medical worldview to focus on deficits (Manago, Davis & Goar, 2017; Shochet et al., 2020), descriptions of autism focused on impairments in social interaction and communication, restricted activities and interests (Di Pietro & Illes, 2014; Ouellette-Kuntz et al., 2006), psychosocial challenges (Shochet et al., 2020), disruptive behaviors (Shochet et al., 2020) and reduced quality of life with potential lifelong implications (Hiebert-Murphy et al., 2008; Lindblom, 2017a). Similarly, autism was associated with “tremendous” (Di Pietro & Illes, 2014, p. 75) or “extraordinary” (Burstyn et al., 2010, p. 125) economic costs for society and families (Leitch, 2007). Despite the propensity for the literature to use the DSM in defining autism, some authors questioned the use of standardized diagnostic assessments with Indigenous children (Di Pietro & Illes, 2014; Lindblom, 2013, 2014a, 2017; Ouellette-Kuntz et al., 2006; Shochet et al., 2020; Woodgate, 2013).
Concerns were raised about the negative impacts of current assessment tools on Indigenous children’s psychosocial wellbeing (Shochet et al., 2020) and their capacity to inform accurate diagnoses and adequate interventions, education and funding for Indigenous child populations (Lindblom 2014a). In this regard, Di Pietro and Illes (2014) expressed caution in using the umbrella term ‘Aboriginal’ for homogenizing the “diverse cultural, social, environmental and linguistic settings of these people...” (p. 75). While Burstyn et al. (2010) noted a five-fold higher prevalence of autism among Indigenous boys than girls in Alberta, no literature attended to differences based on factors such as age, gender, geographical location or Indigenous identity.
Several authors expressed concerns about how negatively stereotyping Indigenous children can contribute to an inaccurate or delayed diagnosis of autism (Di Pietro & Illes, 2014; Hiebert-Murphy et al., 2008)). Shochet et al. (2020) suggested that the deficit nature of the DSM diagnostic criteria for autism and Indigenous views that do not perceive neurodiversity as a ‘disability’, contributed towards a low prevalence of Indigenous children identified with this diagnosis in Canada. Shochet et al. (2020) also posited that the use of the DSM diagnostic criteria does not align with Indigenous views more broadly on neurodiversity.
Select articles did explicitly highlight differences in understandings and definitions of disability, frequently contrasting Western and Indigenous worldviews (Di Pietro & Illes, 2016; Lindblom 2017; Shochet et al., 2020; Stephanow, 2019; Inman, 2019). Stephanow (2019) alluded to Indigenous perspectives in which child wellbeing is embedded in land, family and community across generations and in which a child with autism can be perceived as being born with a ‘special gift’. Lindblom (2013) noted that “ethnical and cultural factors may affect the extent to which Aboriginal children are diagnosed with autism” (p. 4), citing the impacts of ‘ethnic bias’, historical oppression and diagnostic substitution of autism symptoms as key factors. Lindblom (2017a) referenced the need for increased research on cultural diversity and autism to inform the delivery of ‘culturally-sensitive’ music interventions for Indigenous children with autism in BC.
In terms of research involving Indigenous perspectives and experiences, three of the 19 studies reviewed, recruited Indigenous adult participants (Di Pietro & Illes, 2016; Hiebert-Murphy et al., 2008; Woodgate, 2013). Research by Woodgate (2013) included 10 Indigenous community members and 10 Indigenous knowledge holders, and a study by Di Pietro and Illes (2016) included four Indigenous health researchers and policy-makers among eight participants. However, in the study by Hiebert-Murphy et al. (2008), only one out of 72 participants were identified as having Indigenous ancestry. Other publications included Indigenous perspectives through community engagement forums (Luckow, 2019; Manitoba First Nations Engagement, 2017; Stephanow, 2019). Lindblom’s doctoral research was the only study found to involve a small number of five Indigenous children with autism (Lindblom, 2017).
Decontextualized and individualistic perspectives that are characteristic of a medical worldview, obscure how Indigenous families and children’s everyday lives are shaped by broader social, economic, colonial and political factors that are often beyond their immediate environment and control (Gerlach et al., 2017). Colonization was identified in some of the literature as a possible contributing factor to the lack of data (Di Pietro & Illes, 2014, 2016; Lindblom, 2013, 2014b, 2017a, 2017b; Shochet et al., 2020). Several authors described the “historical impact of colonialism” (Di Pietro & Illes, 2016, p. 243) and a “history of oppression and colonization” (Shochet et al., 2020, p. 2). Only Lindblom (2017a) framed “the historical trauma of colonialism” as being “still very much present” in Indigenous peoples’ lives (p. 272) and raised concerns about an autism diagnosis becoming just another label (Lindblom, 2014a).
The Invisibility of Indigenous Children with Autism
An additional prominent theme in the literature was a lack of data on the prevalence of Indigenous child populations with autism in Canada (Burstyn et al., 2010; Di Pietro & Illes, 2014, 2016; Inman, 2019; Lindblom, 2013; Lindblom, 2014a, 2014b; Ouellete-Kuntz et al., 2006; Shochet et al., 2020). Indeed, the Canadian government recommended that children’s ‘ethnicity’, which was not captured in their 2018 ‘National Autism Surveillance System’, needs to be included in this system in the future. No mention was made about Indigenous children.
Currently, as Shochet et al., (2020) stated, the “prevalence of autism [in Indigenous populations in Canada] is largely unknown” (p.2). In their examination of over 200,000 provincial health records between 1998 and 2004, Burstyn et al. (2010) identified lower rates of Indigenous children with a diagnosis of autism and a later median age of diagnosis (five versus three years of age) compared to non-Indigenous children. Several papers questioned whether the apparent under-representation of Indigenous children with autism was linked with the over diagnosis of Indigenous children with FASD (Di Pietro & Illes, 2014, 2016; Leitch, 2007; Shochet et al., 2020). Authors questioned whether this pattern was associated with Indigenous communities’ lacking awareness about autism (Di Pietro & Illes, 2014, 2016), a lack of autism specific services and resources (Manitoba First Nations Engagement, 2017; Shochet et al., 2020) or an overlap between the diagnostic criteria for autism and FASD (Inman, 2019). Pietro and Illes (2016) highlighted that a lack of autism data and the propensity of FASD data risked perpetuating negative, racialized stereotypes and discriminatory practices. These authors also cautioned against assuming that the absence of epidemiological data on autism signified that autism is indeed absent or lower among Indigenous child populations (Di Pietro & Illes, 2014).
A noticeable theme in the literature was the need for effective coordination among national data collection agencies and research, including greater capacity to inform autism policy and research priorities and decisions about funding and service delivery with Indigenous populations (Canadian Autism Partnership Project, 2016; Leitch, 2007; Burstyn et al., 2010; Di Pietro & Illes, 2016; Lindblom, 2014a, 2013, 2017b; Shochet et al., 2020; Ouellette-Kuntz et al., 2006). Concerns about how a lack of accurate data on Indigenous children with autism in Canada creates health inequities was raised in 2016 by the Canadian Autism Partnership Project and four years later by Shochet and colleagues (2020), who highlighted the need to identify the prevalence and experiences of Indigenous peoples with autism in order to understand and address the known gaps in services.
The Complexity of Navigating the Autism System
The literature identified various types of health and educational services and supports for Indigenous children with autism, including early intervention in the form of occupational therapy and physiotherapy (Di Pietro & Illes, 2016), psychosocial services (Di Pietro & Illes, 2016; Shochet et al., 2020), school-based support services (Stephanow, 2019) and behavioral interventions (Inman, 2019). Lindblom (2013, 2014b, 2017a, 2017b) exclusively focused on the provision of music therapy to facilitate Indigenous children’s social inclusion in their communities. Furthermore, in a review of literature on psychosocial resources developed and trialled with Indigenous peoples with autism, Shochet et al. (2020) claimed that “all articles showed some promising findings for improving psychosocial wellbeing for Indigenous children with ASD” (p. 1).
The Canadian Autism Partnership Project (2016) highlighted the need for a significant increase in resources and services that reflect the ‘cultural values’ and needs of Indigenous children and families with autism in this country. Similarly, reports published by the Manitoba First Nations Engagement (2017) and Woodgate (2013) called for the full implementation of Jordan’s Principle in order to address the needs of Indigenous children with extra support needs. In research studies described by Stephanow (2019) and Luckow (2019), partnerships were formed with Indigenous communities and Elders to identify perceived gaps, needs and improvements in autism services for children. However, in the remaining literature, there was a notably lack of literature on distinct Indigenous views and approaches to supporting children with autism and their families.
A recurring theme in the reviewed literature was how the complexity involved in accessing autism systems and obtaining a timely diagnosis and funding for services and supports, including early intervention, was a significant deterrent for many Indigenous communities and parents (Canadian Autism Partnership Project, 2016; Di Pietro & Illes, 2014, 2016; Hiebert-Murphy et al., 2008; Luckow, 2019; Lindblom 2014a; Woodgate, 2013; Manitoba First Nations Engagement, 2017; Shochet et al., 2020). In response, some of the literature pointed to the need for Indigenous communities to have increased awareness about autism by initiating ‘awareness campaigns’ to ensure appropriate delivery of programs and services (Government of Canada, 2018; Manitoba First Nations Engagement, 2017; Woodgate, 2013).
Structural challenges identified in the literature as contributing towards underdiagnosis, and delays in access to appropriate and timely diagnostic and support services, included a mis-diagnosis of FASD (Manitoba First Nations Engagement, 2017; Inman, 2019; Pietro & Illes, 2016), concerns about negative stereotyping and discrimination (Lindblom 2014, Di Pietro & Illes, 2016; Shochet et al., 2020), and living in a rural First Nation (Ouellette-Kuntz et al., 2006; (Burstyn et al., 2010; Di Pietro & Illes, 2016; Lindblom, 2014b). Other factors shaping the extent to which Indigenous children were being diagnosed with autism, included ethnicity, culture and gender (Lindblom, 2017a; Woodgate, 2013). Poverty was also raised as a possible contributing factor to low rates of Indigenous children being diagnosed with autism (Burstyn et al., 2010; Di Pietro & Illes, 2014, 2016). Inequities in funding for First Nations children with autism living on reserve was identified as a prominent structural barrier before (Ouellette-Kuntz et al., 2006) and following the launch of the Jordan’s Principle inspired Child First Initiative by the federal government in 2016 (Inman, 2019; Lindblom, 2017b; Stephanow, 2019; Manitoba First Nations Engagement, 2017).
One of the research questions guiding this scoping review was ‘What is known about the intersections of autism, the child protection system in Canada and Indigenous communities? Only Di Pietro and Illes (2016) and the Manitoba First Nations Engagement (2017) report raised concerns about the relationship between the autism and child welfare systems; noting that Indigenous children with neurodevelopmental disorders, including autism, are often placed and remain in foster care because their communities and/or families lack access to appropriate resources and services. The authors of the report noted that “federal funding dollars for First Nations is inadequate... amount[ing] to discrimination, the outcome of which is higher rates of poverty and increased child apprehension rates” (p. 30). Among several recommendations, the Manitoba First Nations Engagement (2017) report called for “changes to justice system practices to include restorative justice options... [and] a new funding model to support a model of care based on prevention, reunification and strengthening of families” (p. 31). Similarly, Di Pietro and Illes (2016) called for increased research and funding to support Indigenous families in safely caring for their children at home.
The Tendency to Research on, not With Indigenous Families and Children
A final recurring and inter-related theme that has significant implications for the design and delivery of an autism system with Indigenous communities, families and children, was the lack of autism research in Canada that was led or authored by Indigenous researchers, and/or centred on the perspectives and experiences of Indigenous children and adults with lived experiences of autism or disabilities more broadly (Di Pietro & Illes, 2014, 2016; Inman, 2019; Lindblom, 2014a, 2017b; Shochet et al., 2020).
A prominent priority in the literature was the adoption of strengths- and community-based practices to improve the engagement of Indigenous peoples in research and epidemiological data on all forms of childhood disabilities including Indigenous children with autism in Canada (Di Pietro & Illes, 2014, 2016; Lindblom, 2014a, 2017a; Manitoba First Nations Engagement, 2017; Shochet et al., 2020; Luckow, 2019; Woodgate, 2013; Ouellette-Kuntz et al., 2006). Lindblom (2014a) and Woodgate (2013) noted that research and data collection efforts, as well as diagnostic processes and policy development, should support the authentic, meaningful, and strengths-based engagement of Indigenous families (Lindblom, 2014a; Woodgate, 2013). Woodgate (2013) also calls for future research on autism services that foster equity, promote increased awareness, promote the health of families as a whole. In a later publication, the Canadian Autism Partnership Project (2016), highlighted that research and data collection efforts should be community driven and reflect the perspectives of Indigenous participants in order to have an immediate practical benefit on the needs of Indigenous children with autism.
Discussion
The aim of this scoping review was to identify and critical analyze recurring themes in peer-reviewed and grey literature on autism and autism services with Indigenous families and children in Canada. Following a comprehensive search strategy, only 19 publications met the inclusion criteria. The following section discusses the practice and research implications for Indigenous families and service providers of the findings of this scoping review and related to our three research questions.
Problematizing the Current Autism System
Colonization and racism can manifest in many ways, including in the taken-for-granted view that certain knowledges are inherently superior to others (Gandhi, 2007). Despite calls to further advance the social model of disability in order to address inequities experienced by disabled children and their families (Dowling & Dolan, 2001), the reviewed literature highlighted autism supports and services that align with a dominant medical worldview (Ouellette-Kuntz et al., 2006; Lindblom, 2013; Di Pietro & Illes, 2016; Inman, 2019; Shochet et al., 2020). The reproduction of a medical worldview of autism and autism services emphasizes a largely decontextualized, individualistic, ableist, and deficit-oriented worldview of autism. Indeed, the medical model of disability is something that social and critical disability scholars have critiqued for decades in an effort to promote a greater focus on the social and cultural production of disability (Oliver, 2013). This hegemonic worldview is problematic in a colonial state such as Canada, as it tacitly colludes with and perpetuates harmful, racializing, and inferiorizing colonial myths and narratives about Indigenous parenting and developmentally ‘at risk’ Indigenous children (Ineese-Nash, 2020; Ineese-Nash et al., 2018; Inman, 2019). From this critical perspective, the findings on the absence of data on Indigenous children with autism and the repeated references to, or inclusion in studies of Indigenous children with FASD (Di Pietro & Illes, 2014, 2016; Leitch, 2007; Shochet et al., 2020; Lindblom 2014) are particularly troublesome given the prevailing misconception and ‘colonial myth’ that FASD is ‘epidemic’ among Indigenous peoples despite evidence to the contrary (Hunting & Browne, 2012; Inman, 2019; Tait, 2009). Using an intersectionality approach, this also highlights the insidious nature of the combined influence of ableism and racism (DeMatthews, 2020). As noted in several studies, a prevailing, stigmatizing discourse was associated with Indigenous children being misdiagnosed with FASD and preventing Indigenous children with autism from obtaining accurate diagnoses, timely services, supports and funding (Di Pietro & Illes, 2014, 2016; Inman, 2019; Manitoba First Nations Engagement, 2017).
While general prevalence data and public awareness regarding autism have risen globally, more specific prevalence rates related to Indigenous children with autism remain absent (Di Pietro & Illes, 2016; Lindblom, 2014b; Shochet et al., 2020). As several studies alluded to, the under-and/or mis-diagnosis of autism with Indigenous child populations in this country may result from their parents’ reluctance to, and/or difficulty in accessing an often-complex system as a result of multifaceted structural barriers (Di Pietro & Illes, 2014; Hiebert-Murphy et al., 2008; Inman, 2019; Lindblom 2014a; Shochet et al., 2020, Manitoba First Nations Engagement, 2017). However, there was limited attention paid to the relationship between the autism and child welfare systems, and the ongoing removal of Indigenous children from their families and home communities in order to access autism supports and services that were not otherwise available/accessible (Di Pietro et al., 2016; Manitoba First Nations Engagement, 2017). Research on the prevention of Indigenous children with autism from entering the child welfare system is urgently needed.
Re-centering Indigenous Knowledges and Transforming the System
The need to adapt or tailor autism services for Indigenous populations was raised (Canadian Autism Partnership Project, 2016; Stephanow, 2019; Di Pietro & Illes, 2014; Manitoba First Nations Engagement, 2017; Ouellette-Kuntz et al., 2006). However, a clear finding in the extant literature, and similar to research in other settler-colonial nations (Bailey & Arciuli, 2020; Bennett & Hodgson, 2017; Bent et al., 2015; Roy & Balaratnasingam, 2010; Wilson & Watson, 2011), was the ongoing subjugation of Indigenous knowledges, perspectives and lived experiences to inform autism services by and with Indigenous families and children (Di Pietro & Illes, 2014; Lindblom, 2014a; Shochet et al., 2020). This subjugation may be viewed as a consequence of the unquestioned hegemony of a medical worldview of autism that is presented as a universal truth and applicable for everyone and the denial of sociological ways of thinking about disability (Oliver, 2013).
Rather than focusing on disability language and concepts, Indigenous communities and health organizations share a desire to focus on a relational process of wellbeing and healing (Métis National Council, 2017; Tagalik, 2015). Ideological differences towards neurodiverse children may further complicate Indigenous parents’ decision-making about accessing a medical diagnosis and system with their children (Ineese-Nash et al., 2018). These findings point to a tension about integrating Indigenous knowledges into tailored services for Indigenous families and children within a dominant autism discourse and system versus investing in Indigenous governed, designed and delivered programs that centre local Indigenous knowledges and respond to families and children’s strengths and priorities. As noted in discussions with co-author Watts , when service providers who are Indigenous deliver services to children with autism and their families, there is a “shared understanding of the past where you don’t have to worry about saying the ‘wrong’ thing. It’s a different relationship” (personal communication, April 21, 2021).
Greenwood and deLeeuw’s (2018) scholarship can be used to further discuss the findings from this review. In their analysis of the early years system in BC, these scholars state:
“All programs and services destined to impact any life quadrant of Indigenous children, youth, families, and communities must grapple with how to be places of transformation. They must devise and initiate and implement anti-colonial strategies that contradict the norms perpetuated by coloniality and an inherently racist system” (p. 13).
Given the authors’ critical analysis of the findings in this scoping review, they contend that the current autism system in Canada needs to be radically transformed in order to ensure that Indigenous and other racialized child populations with autism in this country have equitable chances to achieve optimal wellbeing and quality of life. This perspective contrasts sharply with the calls in the reviewed literature to focus on ‘awareness campaigns’ in order to address concerns about the apparent under-diagnosis of Indigenous children with autism and mitigate the complexity of the autism system (Government of Canada, 2018; Manitoba First Nations Engagement, 2017; Woodgate, 2013). The authors posit that Indigenous-led approaches are likely more beneficial than focusing on ‘awareness campaigns’ about medically-centric autism programs and services (Government of Canada, 2018; Manitoba First Nations Engagement, 2017; Woodgate, 2013).
The findings are also highly pertinent for questioning how Jordan’s Principle and other funding for services with neurodiverse Indigenous child populations do not inadvertently perpetuate the subjugation of Indigenous knowledges and rights and maintain the status quo of a complex autism system. Indigenous-led transformation upholds the rights of Indigenous peoples to be self-determining in caring for their families and children, advances the implementation of the UN Declaration of the Rights of Indigenous Peoples (United Nations, 2007), and the Calls to Action of the Truth and Reconciliation Commission (2015). The principles underpinning the recent national Indigenous Early Learning and Child Care Framework (Government of Canada et al., 2018) may provide a starting point for a transformative autism system that 1) centre Indigenous Knowledge(s), Languages, and Cultures, 2) upholds First Nations, Inuit, and Métis rights to determination, 3) creates culturally-appropriate quality programs and services, 4) supports child- and family-centredness, 5) responds to children’s families and communities diverse abilities, geographical locations and socio-economic circumstances; 6) supports flexible programs and services, 7) is accessible for all families and children, 8) is designed, delivered and funded with transparency and accountability, and 9) strengthens respectful partnerships and collaborations at multiple levels and across sectors.
Advancing Indigenous Data Governance and Research
Centering Indigenous knowledges and understanding the priorities and needs of Indigenous parents raising neurodiverse children is limited by a severe lack of research (Gerlach, 2018), and particularly research undertaken by Indigenous peoples. “Without research that is led and informed by Indigenous peoples – the wrong questions can get asked which can translate into knowledge that does not benefit Indigenous families or children” (Watts, personal communication, April 21, 2021). Currently, the national data collection agency, Statistics Canada, do not collect any data on the number of racialized and/or Indigenous children with disabilities in Canada, under the age of 15 years. However, information on Indigenous peoples with disabilities over the age of 15 is provided (Statistics Canada, 2019). As this review highlights, the current lack of accurate data on the prevalence of autism among Indigenous children in Canada contrasts with the increasing prominence and incidence of autism in the general child population in this country (Public Health Agency of Canada, 2018). This lack of data and research results in a paucity of evidence to fund, inform and deliver effective and culturally safe disability services with Indigenous children and their families (Gerlach, 2018), and mask or contribute towards serious social and child health inequities (Greenwood et al., 2020). This paper highlights the need for Indigenous-led research and Indigenous governance of data collected about and used for the benefits of neurodiverse Indigenous children and their families. Having a central and accessible repository for this data and research is also essential in supporting the advancement of Indigenous designed and delivered services for Indigenous families seeking information and supports for children with autism.
Limitations
There are several limitations associated with our scoping review. Scoping reviews of literature ‘cast a broad net’ so as to have a wide data capture. In capturing such breadth of evidence, there is no measure or grading of research quality. Some scholars suggest that not grading research evidence has implications for the quality of the research studies reviewed. Covid-19 delayed the conduct of research at our university and slowed the process of data retrieval. Although we made efforts to compile a diverse research team, only one member is Indigenous identifying. More efforts should be made to garner Indigenous leadership on research projects in the future.
Conclusion
We conducted a critical scoping review on Indigenous children living with autism and their use of autism services in Canada. Our review was informed by eclectic critical theories to bring a lens that is attentive to power imbalances and assumptions in the literature. Our findings illuminated the hegemony of medical worldviews in the care of children with autism, a lack of data on Indigenous children with autism that renders them invisible, the grave challenge and complexity of navigating the autism system, and a tendency for research to be conducted on Indigenous children rather than with Indigenous children. Indeed, such as on versus with approach reproduces the colonial relations that Indigenous people have been exposed to for decades. Future research that is grounded in Indigenous rights, relationality, and Indigenous worldviews are needed, with specific attention to the confluence of ableism and racism in the care and treatment of children with autism. Specifically, programs and services for Indigenous autistic children and families should be developed that are rooted in sociological understandings of disability, relationality, and Indigenous rights to self-determination.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This work was financially supported by the receipt of an internal grant in the Faculty of Human and Social Development at the University of Victoria by the lead author.
Endnotes
- The term ‘parents’ in this paper is inclusive of children’s primary caregivers/guardians, including birth and foster parents and extended family members. Similarly, use of the term ‘family’ recognizes the diversity inherent in family structures and is inclusive of a broad understanding of ‘parents’
- Hegemony, as a way of thinking, occurs when a dominant group’s vision of reality is taken up uncritically as a ‘commonsense’ ideology that is applied and taken up universally (Gramsci, 1978).
References
- Allan, B., & Smylie, J. (2015). First peoples, second class treatment: The role of racism in the health and well-being of Indigenous peoples in Canada. Retrieved June 5, 2015 from http://www.wellesleyinstitute.com/wp-content/uploads/2015/02/Report-First-Peoples-Second-Class-Treatment-Final.pdf
- American Psychiatric Association (2013). Diagnostic and statistical manual of mental disorders: DSM-5. 5th ed. Arlington: American Psychiatric Association.
- Arksey, H., & O'Malley, L. (2005). Scoping studies: towards a methodological framework. International Journal of Social Research Methodology, 8(1), 19-32.
- Bailey, B., & Arciuli, J. (2020). Indigenous Australians with autism: A scoping review. Autism, 24(5), 1031–1046.https://doi.org/10.1177/1362361319894829
- Bennett, M., & Hodgson, V. (2017). The missing voices of Indigenous Australians with autism in research. Autism, 21(1), 122–123. https://doi.org/10.1177/1362361316643696
- Bent, C. A., Dissanayake, C., & Barbaro, J. (2015). Mapping the diagnosis of autism spectrum disorders in children aged under 7 years in Australia, 2010–2012. Medical Journal of Australia, 202(6), 317–320. https://doi.org/10.5694/mja14.00328
- Burstyn, I., Sithole, F., & Zwaigenbaum, L. (2010). Autism spectrum disorders, maternal characteristics and obstetric complications among singletons born in Alberta, Canada. Chronic Diseases and Injuries in Canada, 30(4), 125–134. https://doi.org/10.24095/hpcdp.30.4.04
- Canadian Autism Partnership Project (2017). Better together: The case for a Canadian autism partnership. Kanata, ON: Available from: http://www.capproject.ca/ images/pdf/CAPP_Executive_Summary_EN.pdf
- Chiarotti, F., & Venerosi, A. (2020). Epidemiology of autism spectrum disorders: a review of worldwide prevalence estimates since 2014. Brain Sciences, 10(5), 274.
- Clarke, V., & Braun, V. (2017). Thematic analysis. The Journal of Positive Psychology, 12(3), 297–298. https://doi.org/10.1080/17439760.2016.1262613
- Crenshaw, K. W. (1991). Mapping the margins: Intersectionality, identity, politics, and violence against women of color. Stanford Law Review, 43(6), 1241-1299.
- Dowling, M., & Dolan, L. (2001). Families with children with disabilities – inequalities and the social model. Disability & Society, 16(1), 21-35. https://doi.org/10.1080/713662027
- DeMatthews, D. (2020). Addressing racism and ableism in schools: A discrit leadership framework for principles. The Clearing House: A Journal of Educational Strategies, Issues, and Ideas, 93, 1, 27 – 34.
- Di Pietro, N. C., & Illes, J. (2014). Disparities in Canadian Indigenous health research on neurodevelopmental disorders. Journal of Developmental and Behavioral Pediatrics, 35(1), 74–81. https://doi.org/10.1097/DBP.0000000000000002
- Di Pietro, N., & Illes, J. (2016). Closing gaps: Strength-based approaches to research with aboriginal children with neurodevelopmental disorders. Neuroethics, 9(3), 243–252. https://doi.org/10.1007/s12152-016-9281-8
- Ellis, L. A., Augustsson, H., Grødahl, A. I., Pomare, C., Churruca, K., Long, J. C., Ludlow, K., Zurynski, Y. A., & Braithwaite, J. (2020). Implementation of e-mental health for depression and anxiety: A critical scoping review. Journal of Community Psychology, 48(3), 904–920. https://doi.org/10.1002/jcop.22309
- Finkelstein, S., Sharma, U., & Furlonger, B. (2021). The inclusive practices of classroom teachers: A scoping review and thematic analysis. International Journal of Inclusive Education, 25(6), 735–762. https://doi.org/10.1080/13603116.2019.1572232
- Gandhi, L. (2007). Postcolonial theory and the crisis of European man. Postcolonial Studies, 10(1), 93-110. https://doi.org/10.1080/13688790601153180
- Gerlach, A. J., Browne, A. J., & Greenwood, M. (2017). Engaging Indigenous families in a community-based early childhood program in British Columbia, Canada: A cultural safety perspective. Health & Social Care in the Community, 25(6), 1763-1773. https://doi.org/10.1111/hsc.12450
- Gerlach, A. J., Browne, A. J., Sinha, V., & Elliott, D. (2017). Navigating structural violence with Indigenous families: The contested terrain of early childhood intervention and the child welfare system in Canada. International Indigenous Policy Journal, 8(3). https://doi.org/10.18584/iipj.2017.8.3.6
- Gerlach, A. J., Teachman, G., Laliberte Rudman, D., Huot, S., & Aldrich, R. (2017). Expanding beyond individualism: Engaging critical perspectives on occupation. Scandinavian Journal of Occupational Therapy, 25(1), 35-43. https://doi.org/10.1080/11038128.2017.1327616
- Government of Canada (2018). Autism spectrum disorder among children and youth in Canada 2018: A report of the national autism spectrum disorder surveillance system. Retrieved from: www.canada.ca/en/public-health/services/publications/diseases-conditions/autism-spectrum-disorder-children-youth-canada-2018.html
- Government of Canada, Assembly of First Nations, Inuit Tapiriit Kanatami, & Métis National Council. (2018). Indigenous early learning and child care framework. https://www.canada.ca/en/employment-social-development/programs/indigenous-early-learning/2018-framework.html
- Gramsci, A. (1978). Selections from political writings 1921-1926. Quentin Hoare.
- Greenwood, M., de Leeuw, S., & Lindsay, N. (2018). Challenges in health equity for Indigenous peoples in Canada. The Lancet, 391(10131), 1645-1648.
- Greenwood, M., Larstone, R., Lindsay, N., Halseth, R., & Foster, P. (2020). Exploring the data landscapes of First Nations, Inuit, and Metis children’s early learning and childcare. https://issuu.com/nccah-ccnsa/docs/rpt-fnim-_elcc-greenwood-en-80pgs-web_niva_2020-11
- Halseth, R., & Greenwood, M. (2019). Indigenous early childhood development in Canada: Current state of knowledge and future directions https://www.nccah-ccnsa.ca/docs/health/RPT-ECD-PHAC-Greenwood-Halseth-EN.pdf
- Helou, M. A., DiazGranados, D., Ryan, M. S., & Cyrus, J. W. (2020). Uncertainty in decision-making in medicine: A scoping review and thematic analysis of conceptual models. Academic medicine: Journal of the Association of American Medical Colleges, 95(1), 157.
- Hiebert-Murphy, D., Trute, B., & Wright, A. (2008). Patterns of entry to community-based services for families with children with developmental disabilities: Implications for social work practice. Child & Family Social Work, 13(4), 423–432. https://doi.org/10.1111/j.1365-2206.2008.00572.x
- Hill Collins, P., & Bilge, S. (2016). Intersectionality. Polity Press.
- Hunting, G., & Browne, A. J. (2012). Decolonizing policy discourse: Reframing the 'problem' of fetal alcohol spectrum disorder. Women's Health and Urban Life, 11(1), 35-53. https://tspace.library.utoronto.ca/bitstream/1807/32417/1/11.1_Hunting_Browne.pdf
- Ineese-Nash, N., Bomberry, Y., Underwood, K., & Hache, A. (2018). Raising a child with early childhood dis-ability supports Shakonehya:ra's ne shakoyen'okon:'a G’chi-gshkewesiwad binoonhyag ᑲᒥᓂᑯᓯᒼ ᑭᑫᑕᓱᐧᐃᓇ ᐊᐧᐊᔕᔥᑲᒥᓂᑯᓯᒼ ᑲᐧᐃᔕᑭᑫᑕᑲ: Ga-Miinigoowozid Gikendaagoosowin Awaazigish, Ga-Miinigoowozid Ga-Izhichigetan. Indigenous Policy Journal XXVIII(3).
- Ineese-Nash, N. (2020). Disability as a colonial construct: The missing discourse of culture in conceptualizations of disabled Indigenous children. Canadian Journal of Disability Studies, 9(3), 28–51. https://doi.org/10.15353/cjds.v9i3.645
- Indigenous populations in Canada. Canadian Journal of Disability Studies, 8(4), 227-261.
- Inman, C. E. (2019). Absence and epidemic: Autism and fetal alcohol spectrum disorder in Indigenous populations in Canada. Canadian Journal of Disability Studies, 8(4), 227-261.
- McKenzie, H. A., Varcoe, C., Browne, A. J., & Day, L. (2016). Disrupting the continuities among residential schools, the Sixties Scoop, and child welfare: An analysis of colonial and neocolonial discourses. The International Indigenous Policy Journal, 7(2). https://doi.org/10.18584/iipj.2016.7.2.4
- Moola, F. J., Moothathamby, N., Naganathan, M., Curran, C. J., Yerichuk, D., & McPherson, A. C. (2020). A scoping review of music therapy in the lives of children and youth with disabilities and chronic conditions in non-acute medical and community-based settings: A novel consideration for art therapists? Canadian Journal of Art Therapy, 33(1), 17-28.
- King, W. M., Hughto, J. M. W., & Operario, D. (2020). Transgender stigma: A critical scoping review of definitions, domains, and measures used in empirical research. Social Science & Medicine, 250, 112867. https://doi.org/10.1016/j.socscimed.2020.112867
- Levac, D., Colquhoun, H., & O'Brien, K. K. (2010). Scoping studies: advancing the methodology. Implementation Science, 5(1), 1-9.
- Leitch, K. (2007). Reaching for the Top: A Report by the Advisor on Health Children and Youth, Health Canada (2008). Retrieved from: https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/hl-vs/alt_formats/hpb-dgps/pdf/child-enfant/2007-advisor-conseillere/advisor-conseillere-eng.pdf
- Lindblom, A. (2014a). Under-detection of autism among First Nations children in British Columbia, Canada. Disability & Society, 29(8), 1248–1259. https://doi.org/10.1080/09687599.2014.923750
- Lindblom, A. (2014b). How to listen and give voice to First Nations children in BC, Canada, diagnosed with Autism Spectrum Disorder–ethnography in practice. In American Indigenous Research Association Conference in Pablo Montana, USA, October 10 2014.
- Lindblom, A. (2017a). ‘It gives them a place to be proud’ – Music and social inclusion. Two diverse cases of young First Nations people diagnosed with autism in British Columbia, Canada. Psychology of Music, 45(2), 268–282. https://doi.org/10.1177/0305735616659553
- Lindblom, A. (2017b). Stepping out of the shadows of colonialism to the beat of the drum: The meaning of music for five first nations children with autism in British Columbia, Canada (Doctoral dissertation, University of Eastern Finland). Retrieved from: https://erepo.uef.fi/bitstream/handle/123456789/18038/urn_isbn_978-952-61-2430-8.pdf
- Lord, C., Brugha, T. S., Charman, T., Cusack, J., Dumas, G., Frazier, T., Jones, E. J. H., Jones, R. M., Pickles, A., State, M. W., Taylor, J. L., & Veenstra-VanderWeele, J. (2020). Autism spectrum disorder. Nature Reviews Disease Primers, 6(1), 5. https://doi.org/10.1038/s41572-019-0138-4
- Luckow, D. (2019). Autism study aims to help Indigenous families procure services. Simon Fraser University News. Retrieved from: http://www.sfu.ca/sfunews/stories/2019/04/aboriginal-peoples-supplement/autism-study-aims-to-help-indigenous-families-procure-services.html
- Manago, B., Davis, J. L., & Goar, C. (2017). Discourse in action: Parents’ use of medical and social models to resist disability stigma. Social Science & Medicine, 184, 169-177.
- Masi, A., Dissanayake, C., Alach, T., Cameron, K., Fordyce, K., Frost, G., ... & Eapen, V. (2021). Clinical outcomes and associated predictors of early intervention in autism spectrum disorder: A study protocol. BMJ open, 11(8), e047290.
- Manitoba First Nations Child and Family Services (2017). Keewaywin engagement: Final Report. Retrieved from: https://manitobachiefs.com/wp-content/uploads/2017/11/Final-FNCFS-Reform-Engagement-Report_September-2017.pdf
- Métis National Council. (2017). Métis Nation holistic health/wellbeing framework. http://www.metisportals.ca/healthportal/framework17907.htm
- Oliver, M. (2013). The social model of disability: thirty years on. Disability & Society, 28(7), 1024 - 1036.
- Ouellette-Kuntz, H., Coo, H., Yu, C. T., Chudley, A. E., Noonan, A., Breitenbach, M., Ramji, N., Prosick, T., Bedard, A., & Holden, J. J. A. (2006). Prevalence of pervasive developmental disorders in two Canadian provinces. Journal of Policy and Practice in Intellectual Disabilities, 3(3), 164–172. https://doi.org/10.1111/j.1741-1130.2006.00076.x
- Public Health Agency of Canada. (2018). Autism spectrum disorder among children and youth in Canada 2018: A report of the National Autism Spectrum Disorder Surveillance System https://www.canada.ca/content/dam/phac-aspc/documents/services/publications/diseases-conditions/autism-spectrum-disorder-children-youth-canada-2018/autism-spectrum-disorder-children-youth-canada-2018.pdf
- Roy, M., & Balaratnasingam, S. (2010). Missed diagnosis of autism in an Australian Indigenous psychiatric population. Australasian Psychiatry, 18(6), 534–537. https://doi.org/10.3109/10398562.2010.498048
- Sinha, V., & Wong, S. (2015). Ensuring first nations children's access to equitable services through Jordan's principle: the time to act is now. Paediatrics & Child Health, 20(2), 62-64.
- Schwellnus, H., King, G., & Thompson, L. (2015). Client-centred coaching in the paediatric health professions: A critical scoping review. Disability and Rehabilitation, 37(15), 1305–1315. https://doi.org/10.3109/09638288.2014.962105
- Shochet, I. M., Orr, J. A., Kelly, R. L., Wurfl, A. M., Saggers, B. R., & Carrington, S. B. (2020). Psychosocial resources developed and trialled for Indigenous people with autism spectrum disorder and their caregivers: A systematic review and catalogue. International Journal for Equity in Health, 19(1), 134. https://doi.org/10.1186/s12939-020-01247-8.
- Statistics Canada (2019). Indigenous people with disabilities in Canada: First Nations people living off reserve, Métis and Inuit aged 15 years and older.
- Retrieved from: https://www150.statcan.gc.ca/n1/pub/89-653-x/89-653-x2019005-eng.htm
- Stephanow, C. (2019). New research projects aims to improve autism supports on First Nations. CTV News Regina. Retrieved from: https://regina.ctvnews.ca/new-research-projects-aims-to-improve-autism-supports-on-first-nations-1.4436502
- Tait, C. L. (2009). Simpering outrage during an 'epidemic' of fetal alcohol syndrome. In P. D. Monture & P. D. McGuire (Eds.), First voices: An Aboriginal women's reader (pp. 312-324). Inanna Publications and Education Inc.
- Tagalik, S. (2015). Inuit knowledge systems, Elders, and determinants of health: Harmony, balance, and the role of holistic thinking. In M. Greenwood, S. de Leeuw, N. M. Lindsay, & C. L. Reading (Eds.), Determinants of Indigenous peoples' health in Canada: Beyond the social (pp. 25-32). Canadian Scholars' Press.
- Truth and Reconciliation Commission of Canada. (2015). Honouring the truth, reconciling for the future: Summary of the final report of the Truth and Reconciliation Commission of Canada. http://nctr.ca/assets/reports/Final%20Reports/Executive_Summary_English_Web.pdf
- United Nations (2007). Declaration on the Rights of Indigenous Peoples. Retrieved from: https://www.un.org/development/desa/indigenouspeoples/wp-content/uploads/sites/19/2018/11/UNDRIP_E_web.pdf
- Van der Kleij, F. M., & Lipnevich, A. A. (2021). Student perceptions of assessment feedback: A critical scoping review and call for research. Educational Assessment, Evaluation and Accountability, 33(2), 345–373. https://doi.org/10.1007/s11092-020-09331-x
- Vivanti, G. (2012). Predictors of treatment outcomes in toddlers with autism spectrum disorders. Neuropsychiatrie de l'Enfance et de l'Adolescence, 5(60), S128.
- Webster, F., Bremner, S., Oosenbrug, E., Durant, S., McCartney, C. J., & Katz, J. (2017). From opiophobia to overprescribing: A critical scoping review of medical education training for chronic pain. Pain Medicine, 18(8), 1467–1475. https://doi.org/10.1093/pm/pnw352
- Wilson, K., & Watson, L. (2011). Autism spectrum disorder in Australian Indigenous families: Issues of diagnosis, support and funding. Aboriginal and Islander Health Worker Journal. https://search.informit.org/doi/abs/10.3316/ielapa.670577298035246
- Woodgate, R. (2013). Understanding the disability trajectory of First Nations families of children with disabilities: Advancing Jordan’s Principle. Retrieved from: https://umanitoba.ca/faculties/nursing/research/media/Booklet_June_Summit.pdf
- Wright, A., Jack, S., Ballantyne, M., Gabel, C., Bomberry, R., & Wahoush, O. (2019). How Indigenous mothers experience selecting and using early childhood development services to care for their infants. International Journal of Qualitative Studies on Health and Well-being. https://doi.org/10.1080/17482631.2019.1601486
- Zwaigenbaum, L., Brian, J. A., & Ip, A. (2019). Early detection for autism spectrum disorder in young children. Paediatrics & Child Health, 24(7), 424-432.
Appendix A
Table 1: Summary of Search Strings and Key Words
Population 1 Population 2 Diagnosis Service Type Location child* OR adolescen* OR youth OR teenage* OR family OR families OR caregiver* OR guardian* OR parent* Indigenous OR Aboriginal OR “First Nations" OR Mètis OR Inuit OR "First Peoples" OR "Indigenous Canadians" autism OR autistic OR "autism spectrum disorder" OR ASD OR asperger OR spectrum OR neurodiverse OR neurodivergent OR “pervasive developmental disorder” service* OR social OR health OR community OR support OR education OR "child welfare" OR "child protection" Canada* OR Alberta OR "British Columbia" OR Manitoba OR "New Brunswick" OR "Newfoundland and Labrador" OR "Nova Scotia" OR Ontario OR "Prince Edward Island" OR Quebec OR Saskatchewan OR "Northwest Territories" OR Nunavut OR Yukon